When infected with flu-like viruses, each infected cell produces between 1,000 and 10,000 new viruses and the total number of flu viruses in your body can rise to trillions within a few days. In most people, the immune system wins this war of no small combat numbers within a week or so.
Exercise and other proactive health activity can help minimize the impact of a COVID-19 or any other viral infection. The immune system is amazing at targeting pathogens. For that to happen, immune cells must “find” the pathogen. Since we only have about 1.5 gallons of blood scattered with leukocytes and about 100,000 miles of blood vessels, we can help the random chance that the right immune cells will be in the right area so they can latch onto pathogens by improving blood flow / vasodilation through exercise. The same is true for lymphatic system fluids. Exercise improves those flow rates as well and leads to improved immunosurveillance.
With similar importance, higher blood and lymph flow from light exercise (that does NOT involve deep breathing) while we are sick, even though we just want to lay in bed, can help improve lymphatic flows that activate immune responses within the lymph nodes, remove septic materials when viral cells burst and/or deteriorate as they “birth” new virions; and improved flows may even help remove excess immune system cytokine action / pre-storm by pushing excess cytokines away from highly infected areas.
COVID appears to “predispose patients to thrombotic disease, both in the venous and arterial circulations, due to excessive inflammation, platelet activation, endothelial dysfunction, and stasis (areas of slow circulating blood)”. Common causes of endothelial dysfunction include diabetes, hypertension, smoking, and physical inactivity.
Rest is important; but inactivity, whether it be at home or in a hospital is probably counter to optimal recovery. This is probably intuitive except when we just really want to lay in bed. Conventional wisdom indicates that we feel better when we get light exercise mixed with rest when sick compared to just laying in bed.
A larger initial exposure viral load can cause increased severity because the exponential viral replication reaches much higher levels before the immune system can respond. This results in dramatically greater viral damage. The increased viral presence also tends to activate a more intense immune response which may result in increased systemic damage from the immune response. Reducing viral loads into a variolative or minor infection range can significantly reduce the likelihood of a severe case. A regular regimen of a few cycles of normal daily exercise improves immune response / speed pre-exposure and immediately following exposure to minimize likelihood of illness.
It is possible to minimize severity of illness by slowing the exponential growth of viral load that develops shortly after exposure which helps the adaptive immune response to mature before exponential viral growth becomes extremely large. The innate immune response tends to slow natural infections; and intelligent behavior (such as using viral inactivation substances such as mouthwash, toothpaste, essential oils / breath-mints / breath-strips, zinc, small amounts of ethyl alcohol, etc.), can slow the exponential growth such that B/T cell activation /maturation occurs before exponential growth of antigen becomes large. Mints and essential oils have been recognized as helpful for many centuries, and many modern mouthwashes that kill bacteria and inactivate viruses are now essential oil rather than alcohol based. Swishing fractions of an ounce of high-percentage ethyl alcohol (hard liquor) into the throat area with tickle/minor-irritation every few hours tends to slow viral growth, although once viral damage to the tissues becomes significant, this tends to create further irritation / tissue damage; and larger amounts of ethyl alcohol may negatively impact immune system response, so this tends to be optimal only for very early “tickle” stages of illness. Placing 1/16th of a zinc supplement (nibble off a small piece) and/or a few grains of salt in room temperature or slightly warm water will make the water much more pleasant to drink, which may help you to remain well hydrated. The zinc also seems to have a throat soothing effect (try it) and may have some mild topical protective characteristics and this tends to be effective in both early and later stages of illness. Just a nibble of a zinc mineral supplement and a few grains of salt go a long way and also tend to make water less irritating to the sore throat – thus encouraging increased hydration which is also helpful. Salt water gargling tends to be helpful. Swishing saliva around within the mouth and onto irritated areas helps to keep them moist and in some cases will help mucosal antibodies find and bind to viruses that may be present near the irritated area that is replicating virus. This can be particularly helpful during re-exposures and in later stages of infections where significant virus specific antibodies may be present within the saliva. Histamine responses also tend to increase likelihood of antibody encounters with viruses within mucosal tissues and also help to purge virus from the body through sneeze and runny nose responses.
It is likely that many infections and transmissions can be avoided or minimized through the use of breath-mints / breath strips during and following potential exposure encounters.
When sick, highly aerobic activity can undesirably facilitate virus movement deeper within the airway and into the lungs, yet light exercise such as walking can stimulate blood/lymph flow without resulting the deep respiration that internally spreads virus within the airway. Similarly, fresh air and avoiding rebreathing “sick-room” viral laden air can help avoid spreading the infection within the airway. Perhaps obviously, keeping considerable physical distance from others while enjoying fresh outdoor air will dilute any viral load that might be shedding when sick and wearing masks can help while in careful transit to some wide open personal space containing fresh air.
Could it be that the “power of suggestion” that we may need to be hospitalized is creating sedentary behavior during sickness that is unhelpful?
Either way, go get some exercise!

Also see Safety Information and Immunology and Hospitalized Patient Physical Therapy
Exercise Lowers Risk
From Table 2 of Physical inactivity is associated with a higher risk for severe COVID-19 outcomes, it can be seen that for those who consistently met physical exercise guidelines, 99 were hospitalized, 32 were admitted to the ICU, and 11 out of 48,440 COVID-19 patients died. Actual “real world” rates are lower as it is likely that between the study period 1 January 2020 and 21 October 2020 many people who actually had COVID-19 were not tested and were never identified. Antibody prevalence surveys in late April 2020 estimated that there were between 10 to 50 times more infections than positively identified COVID-19 cases. This would mean the odds of the median person who meets the physical exercise guidelines in the study has between a 1/44,000 to 1/220,000 chance of dying from COVID-19. Comparatively, 760 people who did not meet exercise guidelines died, which means that the median of those not meeting exercise guidelines have a 69 times greater chance of dying. The exercise threshold selected for the study was >150 minutes of “moderate to strenuous / like a brisk walk” exercise per week. Twenty one minutes of exercise per day could be a life-saver. It would be interesting to see data for people who enjoy sports / exercise to the tune of 500 to 1000 minutes per week. Japan has had lower fatalities that may be related to exercise-at-work culture and generally healthy BMI.

Are we immune by chance? “The launch of an immune response can sometimes be predicted by mass action, because collisions have to take place between the pathogens and the cells of the immune system (e.g., Sykulev et al., 1995): the stronger the pathogen attack, the higher the immune reaction, on average. Nevertheless, how rapidly immune cells react will vary by host (Frank, 2002), partly because of variation in the rate at which immune cells patrol through the body (e.g., Lee et al., 2012).”
To clarify, this is not intended to create mystery or the idea that immunity is purely chance. It is intended to show that there are elements of probability in the functioning of the immune system and that increased blood and lymph flow increases those probabilities.


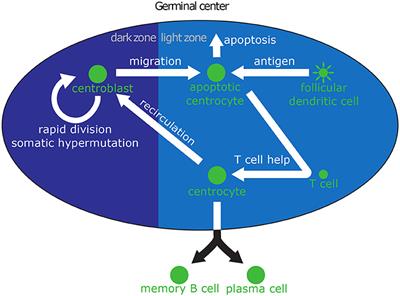

COVID-19 epidemiologists continue to research why clinical infection rates are lower in Japan and other Asian countries. It could be exercise that increases lymph flow such that the virus more rapidly contacts leukocytes in SLO germinal centers such that adaptive immune response is accelerated.


Cytokine storms and sepsis are a major contributor to COVID19 fatalities. This study of mice relates exercise and likelihood of sepsis in studies with mice.

Movement Matters – Pumping the Lymphatic System




“Coronavirus disease 2019 (COVID-19), a viral respiratory illness caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), may predispose patients to thrombotic disease, both in the venous and arterial circulations, due to excessive inflammation, platelet activation, endothelial dysfunction, and stasis.”

Balance: Over-exercising and over-exercising immediately prior to infection / or during symptom development could be counter-productive, as one might intuitively guess. Is it possible that an anecdotal case study of a marathon runner COVID19 fatality was aggravated through extreme exercise sepsis? While this is not known, the negative effects of excessive exercise is explained in this article.



Going one step further, light exercise during early cytokine storm activity or pre-storm could be helpful. Take a walk when you are able. It could be too late during late-storm and sepsis, so it may be better to take that walk even when wanting to lay in bed all day.

Several general articles regarding health. COVID, and the great outdoors.







Perhaps it’s best to get that exercise outdoors where sunlight can generate vitamin D. Vitamin B is also helpful and tends to provide an energy boost. Vitamin C and multivitamins are helpful. Some articles favor megadoses, but meeting RDA levels is a safe recommendation. Essential oils such as peppermint and others found in mouthwash and breath fresheners can be soothing and especially helpful as preventative germicides.

Placing 1/16th of a zinc supplement (nibble off a small piece) and/or a few grains of salt in room temperature or slightly warm water will make the water much more pleasant to drink, which will enable you to remain well hydrated. The zinc also seems to have a throat soothing effect and may have some mild topical protective characteristics. Just a nibble and a few grains go a long way.

It has been well recognized that lying prone / stomach or side is healthier than lying on the back when lungs are being stressed.
Virus Life Cycles, Structure, Senses, Etc.
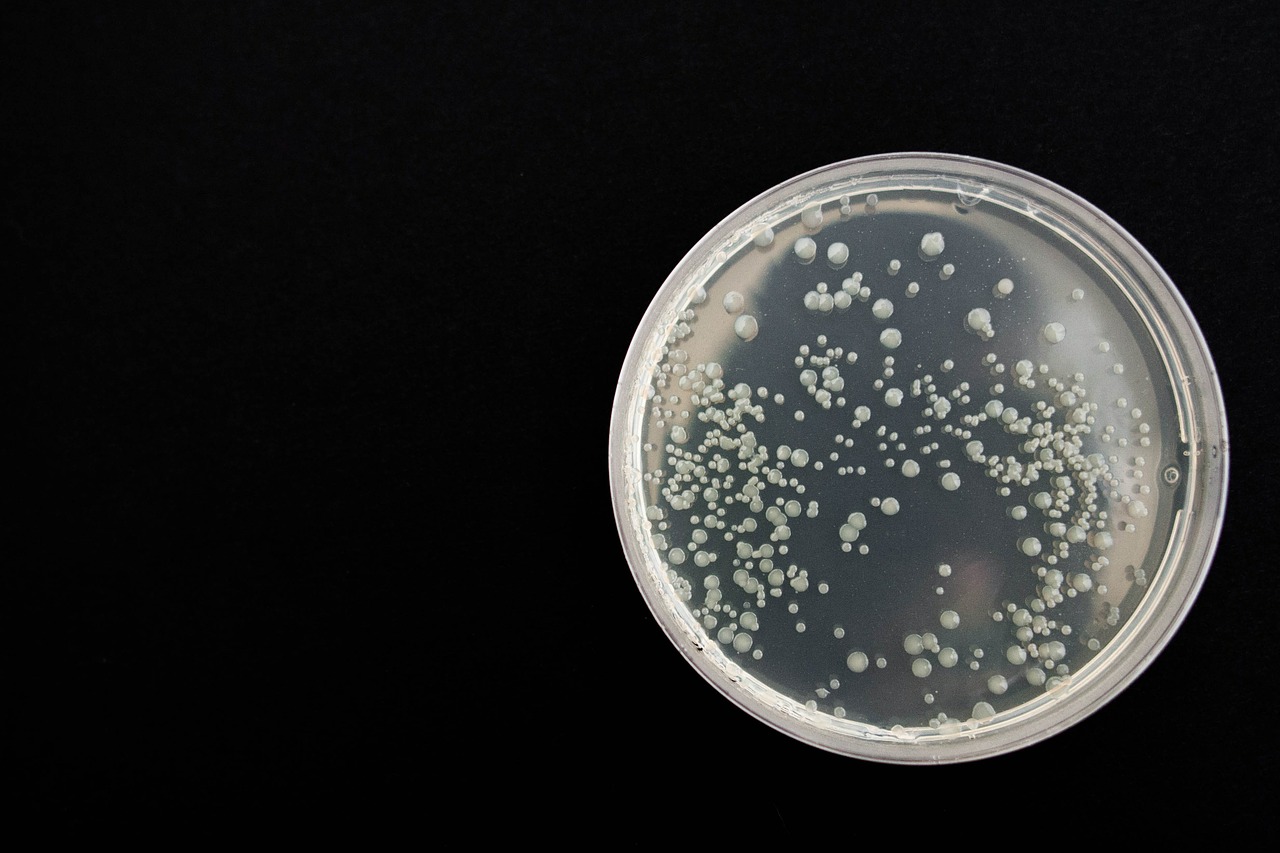

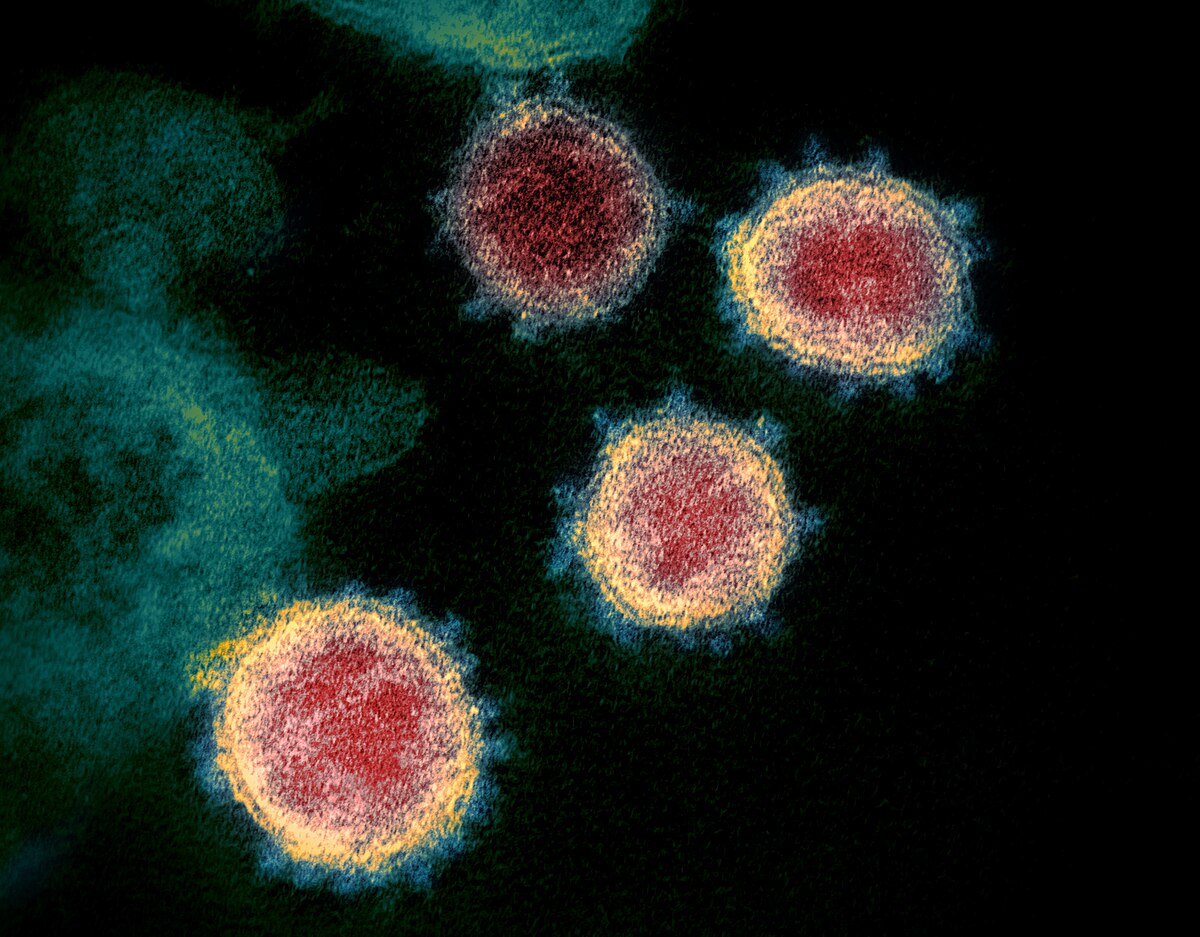
“Viruses can be released from the host cell by lysis, a process that kills the cell by bursting its membrane and cell wall if present. This is a feature of many bacterial and some animal viruses.”
“Budding is [another] method which viruses use to exit the cell. “Budding” through the cell envelope, in effect using the cell’s membrane for the virus itself is most effective for viruses that need an envelope in the first place. These include enveloped viruses such as HSV, SARS, or smallpox.”.
Influenza and SARS-CoV-2 are also enveloped viruses that are released through budding.


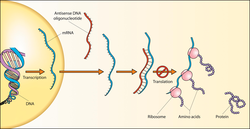
The genome of an RNA virus can be said to be either positive-sense, also known as a “plus-strand”, or negative-sense, also known as a “minus-strand”. In most cases, the terms “sense” and “strand” are used interchangeably, making terms such as “positive-strand” equivalent to “positive-sense”, and “plus-strand” equivalent to “plus-sense”.
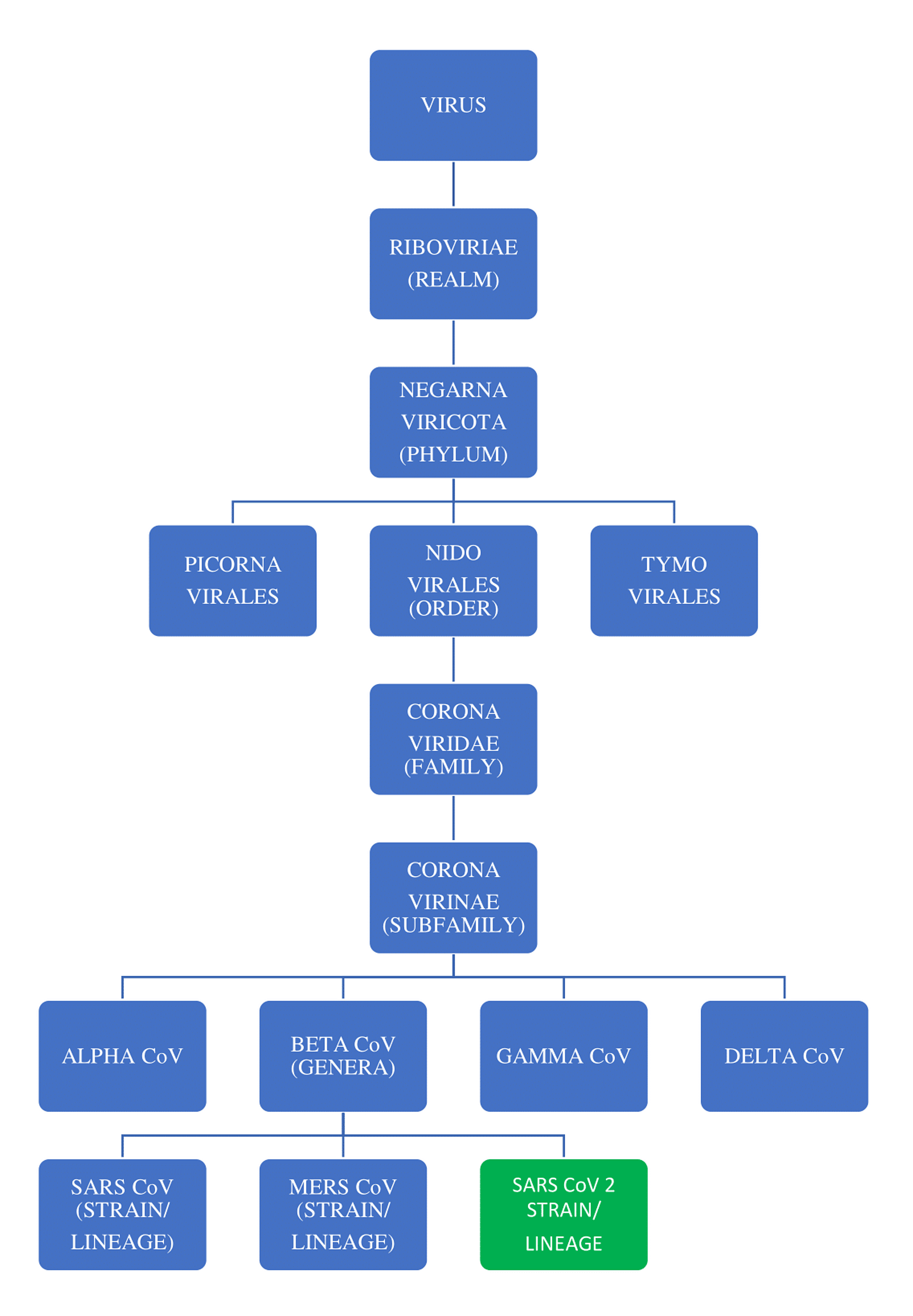
The coronaviruses (CoVs) belong to the genus Coronavirus, the family Coronaviridae, and the order Nidovirales [1]. They are enveloped and have a non-segmented, single-stranded, positive-sense ribonucleic acid (ssRNA+) as their nuclear material. On electron microscopy, these viruses show a characteristic appearance that resembles a crown (corona in Latin means crown) due to the presence of club-shaped surface protein projections [2-3]. The CoVs are pleomorphic, measure between 80 and 160 nm in length, and have a small genome measuring 27-32 Kilobytes (KB) with a unique replication strategy
Viral Replication
“Replication is very quick: after only 6 hours the first influenza viruses are shed from infected cells.”
So imagine multiplying by 1,000 to 10,000, the first of which appear in only 6 hours. That’s what happens until the immune system engages the viruses and begins killing the viruses and the cells they have infected. The innate immune system helps thwart this at the very start, but until the adaptive immune system response matures and scales, viral replication is exponential.


